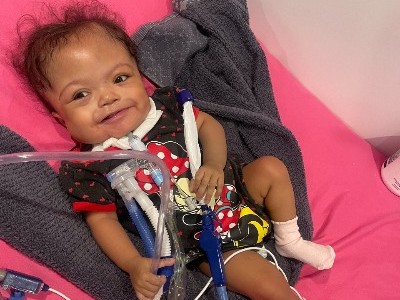
In the realm of pediatric cardiac surgery, stories of resilience and medical innovation frequently emerge, but few resonate as powerfully as that of Ashley Mercedes. Born prematurely at just 28 weeks and weighing a mere 1.1 kilos, Ashley faced an uphill battle from her first breath. Diagnosed with hypoplastic left heart syndrome (HLHS), a severe congenital heart defect, her chances of survival appeared slim. However, thanks to a staged, hybrid surgical strategy pioneered at Children’s National Hospital, Ashley’s story became one of hope and triumph.
At Children’s National Hospital, a team of dedicated specialists utilized an innovative “hybrid strategy” to provide Ashley Vela Mercedes with the crucial time she needed to grow stronger before undergoing open-heart surgery. This staged approach proved to be life-saving for Ashley, allowing doctors to meticulously manage her condition and address any complications that arose. Today, Ashley Mercedes is a vibrant and joyful 18-month-old, a testament to the groundbreaking care she received. Her journey stands as an inspiring example of medical expertise overcoming seemingly insurmountable odds.
Doctors believe Ashley Mercedes holds the distinction of being the smallest infant born at 28 weeks with HLHS to not only survive but thrive to this age. While ongoing care and future procedures remain part of her path, her family is filled with profound gratitude for the exceptional knowledge and unwavering dedication of the medical team at Children’s National. The hybrid program, expertly co-led by cardiac surgeon Dr. Can Yerebakan and interventional cardiologist Dr. Joshua Kanter, played a pivotal role in Ashley’s miraculous recovery.
A Hypoplastic Left Heart Syndrome Miracle: The Ashley Mercedes Story
Ashley Mercedes is more than just a happy, smiling 18-month-old; she embodies a true medical marvel. Her story is a powerful illustration of hope for families facing similar daunting diagnoses. Born prematurely to Ana Mercedes and Axel Vela, Ashley arrived into the world weighing about the same as a beanie baby, with a heart no larger than a grape. The news of Ashley’s premature birth and critical HLHS diagnosis was devastating. Doctors initially painted a bleak picture, suggesting survival was unlikely. For Ana and Axel, who had long dreamed of building a family, this news was shattering. Despair and fear began to overshadow their hopes for their tiny daughter.
Hybrid Procedure: Offering a Lifeline to Ashley Mercedes
Despite the grim prognosis, Dr. Jennifer Lindsey, Ashley’s cardiologist, refused to surrender hope. Seeking innovative solutions, she reached out to the renowned team at Children’s National Hospital to explore the possibility of a “hybrid procedure.” Dr. Lindsey recognized that this novel approach might offer a chance to stabilize Ashley Mercedes‘s heart, providing her precious time to grow and gain strength before enduring the necessary open-heart surgeries that lay ahead.
Hybrid heart procedures represent a groundbreaking fusion of traditional surgical techniques and minimally invasive interventional cardiology, often involving catheter-based approaches. In Ashley’s case, the hybrid procedure involved implanting a stent into her ductus arteriosus. This vital blood vessel, which typically ensures efficient blood flow to the placenta during fetal development and naturally closes after birth, was kept open by the stent. Maintaining the ductus arteriosus in an open state was crucial to enhance blood flow and oxygenation for Ashley.
It’s important to understand that the hybrid procedure is not a permanent solution for HLHS. Instead, it serves as a crucial bridge, granting fragile infants like Ashley Mercedes invaluable time to mature and develop before undergoing the more extensive open-heart surgeries required to reconstruct the heart for long-term function. Hybrid procedures are generally reserved for infants at exceptionally high risk for traditional open-heart surgery, explaining why only a limited number of specialized congenital heart centers worldwide offer this advanced option.
The hybrid team at Children’s National, under the guidance of Drs. Yerebakan and Kanter, stands out for their extensive experience in performing these complex procedures on the most vulnerable infants. Their dedication to innovation led them to collaborate with the U.S. Food and Drug Administration to bring a smaller, more flexible stent from Europe to the United States. This toothpick-sized stent was specifically designed for delicate cases like Ashley Mercedes, enabling more precise and less invasive interventions within the ductus arteriosus.
Record-Setting Hybrid Surgery for Baby Ashley Mercedes
Dr. Gil Wernovsky, a cardiac intensive care specialist at Children’s National and Ashley Mercedes’s cardiologist at the hospital, emphasized the significant challenges Ashley faced from birth. Her initial birth weight of 1.1 kilos (2.4 pounds) was considered too low for immediate surgery, and her lungs were still underdeveloped. For several weeks, Ashley remained under the diligent care of Dr. Lindsey at Inova Children’s Hospital, receiving the critical support necessary to grow and mature to a point where the hybrid procedure became a viable option. Dr. Wernovsky acknowledges the crucial role of the Inova Children’s Hospital team in providing the foundational care that paved the way for Ashley’s subsequent treatment.
Once Ashley Mercedes reached 1.7 kilos (3.7 pounds), she was carefully transferred to the Cardiac Intensive Care Unit (CICU) at Children’s National Hospital for her groundbreaking hybrid procedure. At that time, she became the smallest baby ever to undergo this complex surgery at Children’s National. Following the procedure, the Children’s National CICU became Ashley’s home for almost her entire first year of life, a testament to the intensive and specialized care she required.
“Landing here at Children’s was a blessing because we thought she was going to die. What has happened here is a miracle,” shared Ana Mercedes, expressing her profound relief and gratitude. “I would like to express to Dr. Yerebakan and Dr. d’Udekem (the chief of Cardiac Surgery at Children’s National) my deepest appreciation. What they have accomplished for my daughter is truly incredible, and I will forever be indebted to them for their unwavering efforts.”
Over the ensuing 11 months within the hospital environment, Ashley Mercedes bravely navigated numerous surgeries and catheterizations, along with countless other necessary medical procedures and tests. Her journey was marked by both progress and setbacks, including critical periods when she required extracorporeal membrane oxygenation (ECMO) – an advanced form of life support – to sustain her through particularly challenging times.
Ashley Mercedes Thriving at Home: A Celebration of Life
July 2021 marked a momentous milestone in Ashley Mercedes’s young life – she finally went home for the very first time. Remarkably, she has not required re-hospitalization since her discharge, a testament to the success of her treatments and ongoing care. Her health is meticulously monitored through a collaborative approach involving Dr. Lindsey and the single ventricle monitoring program at Children’s National. This innovative program maintains close virtual contact with families like Ashley’s three times a week, leveraging telehealth to track her growth and development. Ana Mercedes actively participates in this virtual care, sharing videos and photos of Ashley as part of her routine updates to the clinical team, ensuring proactive and responsive care.
While Ashley Mercedes still requires some medical support within her home environment and will likely need further medical interventions in the future, she is, for the present, a thriving, more independent, and demonstrably happier little girl. She stands as an extraordinary testament to resilience – the smallest baby born with HLHS at such a low birth weight to not only survive but flourish to this age.
Ana Mercedes cherishes the dream of one day taking Ashley to the Dominican Republic, her homeland, to experience its beautiful beaches and connect with her heritage. “We are overall doing well. We have received unwavering support from our family and employers,” Ana Mercedes gratefully acknowledges. “We are profoundly thankful to everyone who has extended a helping hand to us during this incredibly challenging journey.”
The past year has been an emotional rollercoaster for the Vela Mercedes family, but Ashley’s progress has been nothing short of extraordinary, surpassing all expectations. Dr. Wernovsky reflects, “Last Christmas, this little girl was undergoing her fourth catheter procedure, having spent her entire life in intensive care. One year later, she is home, surrounded by her loving family, and celebrating – truly a Christmas miracle.” The story of Ashley Mercedes serves as a powerful reminder of the hope that medical innovation and compassionate care can bring, even in the face of the most daunting challenges.